Explore EHN
Your gateway to environmental health knowledge
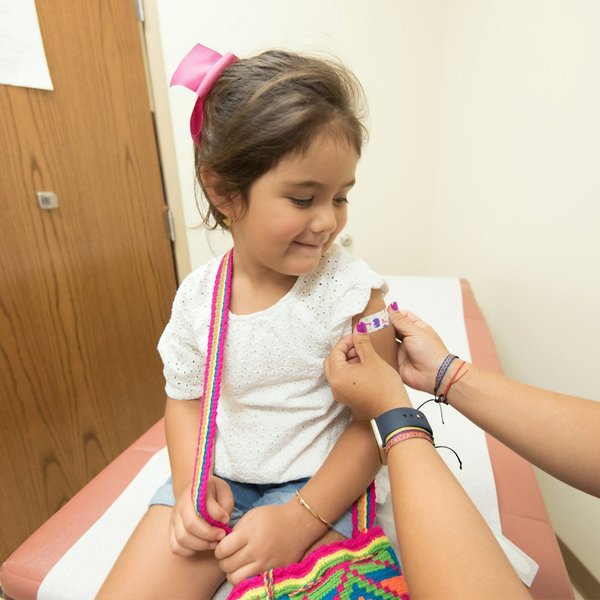
Children’s Health
Consequential reporting about children's health, written and selected by journalists and scientists at Environmental Health News.
Climate
Consequential reporting about our changing climate, written and selected by journalists and scientists at Environmental Health News.
Environmental Health News
Your support of EHN, a newsroom powered by Environmental Health Sciences, drives science into public discussions. When you support our work, you support impactful journalism. It all improves the health of our communities. Thank you!

Top News
The latest environmental health news from across the globe.
Justice
The intricacies of environmental health, encompassing diverse ecosystems, human well-being, and sustainable practices.
Toxics
The intricacies of environmental health, encompassing diverse ecosystems, human well-being, and sustainable practices.
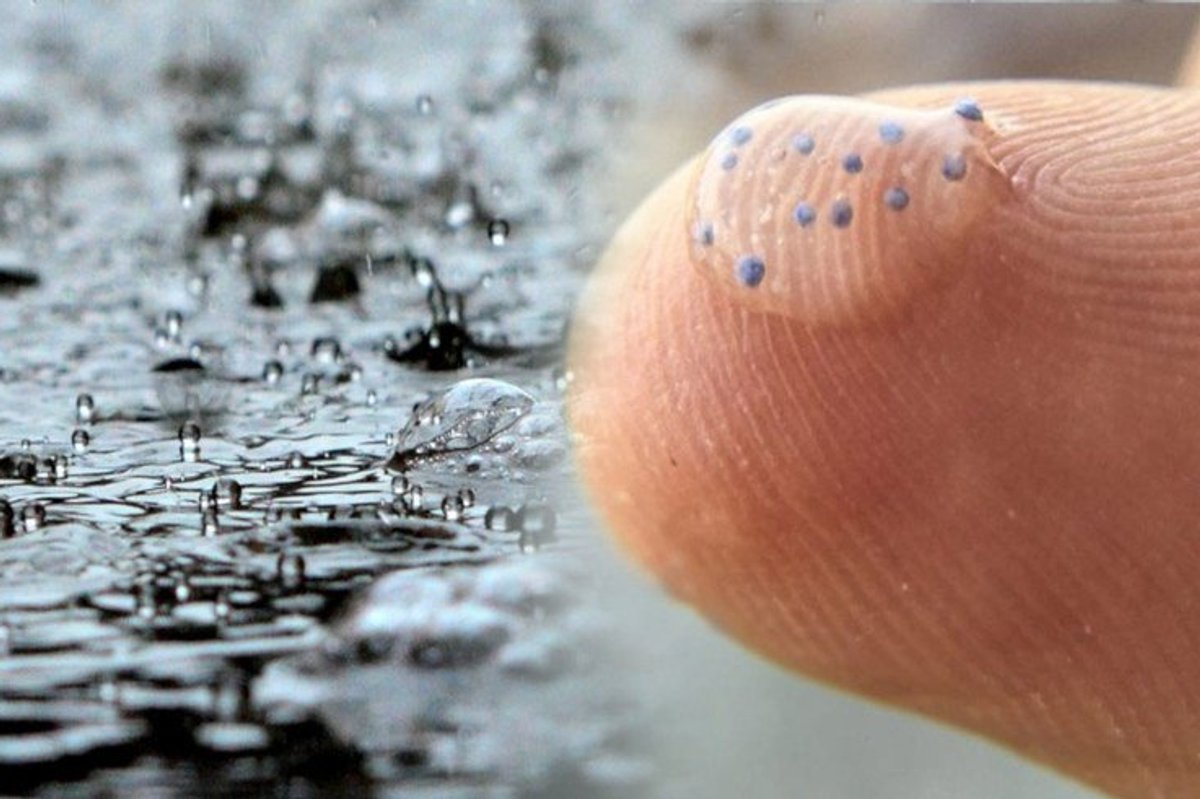
Plastic Pollution
The intricacies of environmental health, encompassing diverse ecosystems, human well-being, and sustainable practices.
Food & Water
Consequential reporting about food and water, written and selected by journalists and scientists at Environmental Health News.